From helping to prevent premature birth, to improving the early detection of serious conditions. Together, these projects are advancing knowledge and care to better protect babies before birth and improve outcomes for families.

Tackling pregnancy complications caused by poor placental function
During pregnancy, the placenta supplies vital oxygen and nutrients to the developing baby. But if it isn’t working properly – known as placental insufficiency – it can cause serious complications that can lead to babies being born too small or too soon. Sadly, this can lead to loss of life or lifelong disabilities.
Dr Viki Male of Imperial College London is investigating the role of a specialised type of immune cell in placental development. Her laboratory research could pave the way to new tests to identify at-risk pregnancies sooner, enabling closer monitoring and timely intervention – improving outcomes for babies and their families.
This project is jointly funded by Action Medical Research and Borne.

Improving diagnosis of a serious heart condition before birth
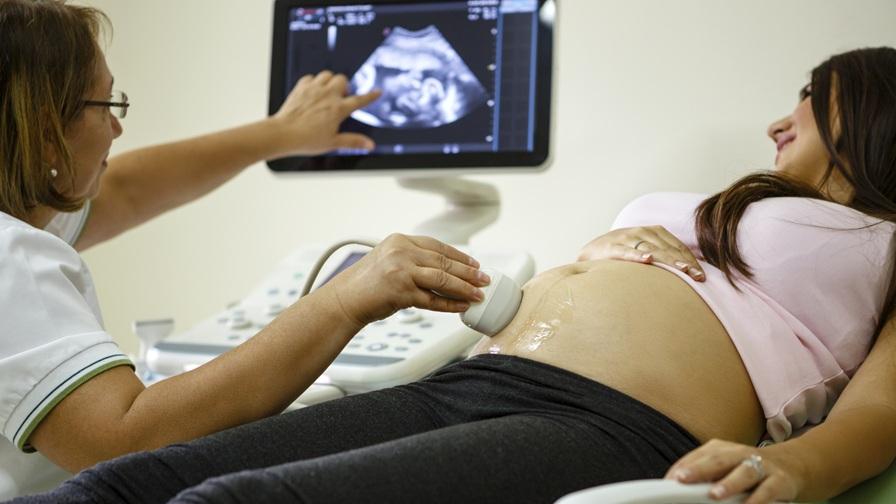
More than 200 babies in the UK are born with coarctation of the aorta (CoA) each year – a condition caused by a narrowing in part of the body’s main blood vessel. Early detection and prompt treatment of severe CoA improves survival and reduces the risk of complications. However, while routine ultrasound scans during pregnancy may suggest its occurrence, the diagnosis is usually only confirmed after birth.
With Action funding, Professor Pablo Lamata of King’s College London is developing a new tool that can reconstruct the 3D shape of the baby’s aorta using routine ultrasound scans. He hopes this will enable earlier, more accurate diagnosis of CoA – reducing uncertainty for families and improving outcomes for babies.
Developing a new tool for earlier, more accurate diagnosis of brain conditions during pregnancy
Each year in the UK around 1,500 pregnancies are affected by conditions where a baby’s nervous system does not form properly. Early and accurate diagnosis of brain malformations is crucial to help parents make informed decisions and to allow doctors to plan the best possible care during pregnancy and following birth.
High-quality fetal magnetic resonance imaging (MRI) can help doctors to identify and better understand abnormalities. But it requires highly trained specialists and is currently only available in a small number of UK hospitals.
Professor Mary Rutherford, at King’s College London, is leading a team developing a new tool to widen access to fetal MRI. By improving image quality, standardising assessments, and producing easy-to-understand reports, this will enable earlier, more accurate diagnosis of brain malformations during pregnancy – supporting better long-term outcomes for children.
Treating epilepsy during pregnancy
An estimated 2,500 children are born to women with epilepsy in the UK each year. While most women have healthy pregnancies, seizures can pose risks to both mother and baby. At the same time, many treatments used to control seizures – including medications and the ketogenic diet – raise concerns because of their potential effects on the developing baby.
At Royal Holloway, University of London, Professor Robin Williams is leading laboratory research to determine whether a new dietary supplement can be safely used to treat epilepsy during pregnancy. This work is an important step towards offering women more options to manage their seizures and protect their unborn babies.
